Have you ever paused before biting into a crisp apple? Maybe you’ve felt a familiar discomfort when laughing heartily in public, worried about loose dentures or a missing tooth showing?
If you’re one of the millions of Americans navigating your senior years, you know that missing teeth can dramatically impact not just your smile, but your everyday quality of life—from how you eat to how you socialize.
The good news? Advances in modern dentistry have made dental implants a highly reliable, long-term solution, and age is rarely a barrier to getting them. In fact, implant procedures are surging among older adults: the largest absolute increase in implant prevalence in the U.S. has been among individuals aged 65 to 74 years old.
If you’re considering this life-changing restoration, here is what you absolutely need to know.
The Major Benefits of Dental Implants for Seniors
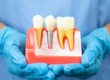
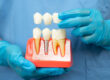
Dental implants, which are titanium posts surgically placed in the jawbone to serve as artificial tooth roots, offer distinct advantages over traditional options such as dentures, especially for older patients.
- Exceptional Success Rates: Implants boast a remarkably high long-term success rate. Studies show that the survival rate of dental implants is often up to 98%, with some research finding a 95.3% survival rate in older adults compared to 93.9% in younger patients. Your age is less of a factor than your overall health.
- Improved Chewing and Nutrition: Implants restore a stable bite, much like natural teeth. This means you can enjoy a wider variety of foods—like steak, nuts, and apples—without discomfort or slippage. A natural, efficient chew supports better nutrition, which is vital for senior health.
- Preservation of Jawbone: When a tooth root is missing, the jawbone underneath begins to deteriorate. Implants stimulate the jawbone, preventing this loss. Long-term data show patients with implants experience less bone loss than those with removable dentures or bridges. This stimulation helps maintain your facial structure and prevents that “sunken” look associated with aging and missing teeth.
- Enhanced Quality of Life: Approximately 96% of people who get dental implants report being satisfied with their results. This improved stability leads to clearer speech and a significant boost in confidence during social interactions.
Medical conditions and surgical risk: what to discuss with your dentist
Seniors commonly have chronic conditions (diabetes, heart disease, COPD) that can affect healing and infection risk. Many of these conditions are manageable during implant therapy, but full disclosure and medical clearance (when appropriate) are essential. Key points your dentist or surgeon will consider:
- Diabetes control: Poorly controlled diabetes raises infection and healing risks — reasonable glycemic control improves implant outcomes.
- Cardiovascular disease & anticoagulants: These affect bleeding risk and peri-operative management; your medical doctor will often advise how to handle blood thinners.
- Cognitive or functional limitations: These impact post-op care and hygiene; caregivers may need to be involved.
A multidisciplinary plan (dentist, primary care physician, and specialists as needed) yields the safest results.
Understanding the Cost and Insurance Coverage
While dental implants in Scottsdale are a significant investment, their longevity often makes them a cost-effective solution over the long term.
Cost Breakdown
The cost of a single dental implant in the U.S. usually includes the titanium post, the abutment (connector piece), and the dental crown. This total price can vary widely depending on your location and whether you require preliminary procedures such as a bone graft or a sinus lift.
The Reality of Medicare
It is crucial for seniors to understand the limitations of federally provided insurance:
- Original Medicare (Parts A & B) does not cover routine dental care, including cleanings, fillings, dentures, or dental implants.
- Your best coverage option is often a Medicare Advantage Plan (Part C). These private insurance plans approved by Medicare usually include additional benefits such as dental, vision, and hearing. Many Part C plans offer coverage or partial reimbursement for dental implants, though benefits vary dramatically, so careful review is essential.
- Alternatively, you can purchase a standalone supplemental dental insurance plan. Many of these plans will cover a portion (e.g., 50%) of major procedures, such as implants, up to an annual maximum benefit.
Are You a Candidate? Key Health Considerations
Age itself is not a contraindication for dental implants. The focus is always on your overall health and the condition of your jawbone.
Your dentist or oral surgeon will assess factors like:
- Bone Density: You need sufficient jawbone to anchor the implant. If you’ve had missing teeth for a long time, bone loss may require a preliminary bone graft.
- Systemic Conditions: Uncontrolled diabetes, certain blood-clotting disorders, and excessive smoking are risk factors that can increase the chance of implant failure. Smokers, for instance, have a 140.2% higher risk of implant failure than non-smokers (Source: National Library of Medicine). Managing these conditions is key to success.
With modern techniques like bone grafting and advancements in guided surgery, healthy seniors can expect exceptional results.
What to expect from the implant process as a senior
The workflow for seniors is the same basic steps as for younger adults, though with more individualized planning:
- Consultation & medical review: Health history, medication list, and imaging (panoramic X-ray, CBCT) to assess bone and anatomy.
- Treatment planning: Decide on the number and position of implants, the need for bone grafting or sinus lifts, and whether immediate loading (same-day crown) is appropriate.
- Surgery & healing: Implant placement is usually performed on an outpatient basis; healing (osseointegration) typically takes a few months before final restoration. Seniors may have slightly longer healing timelines depending on health and bone quality.
- Restoration & follow-up: Crowns, bridges, or implant-supported dentures are attached, and regular maintenance visits are scheduled to check bone levels and hygiene.
Experienced implant teams tailor timeline and techniques (mini-implants, zygomatic implants, short implants, overdentures) to reduce surgery and speed recovery when appropriate.
Benefits vs. tradeoffs for seniors
Benefits:
- Restored chewing ability, improved nutrition, and greater comfort than poorly fitting dentures.
- Higher satisfaction and often improved quality of life compared with removable dentures.
Tradeoffs:
- Higher up-front cost and limited insurance coverage.
- Need for ongoing oral hygiene and regular dental checkups.
- Possible additional procedures (bone grafts) that lengthen treatment time and cost.
For many seniors, the long-term functional and quality-of-life gains outweigh the costs — but it’s a personal decision based on health, finances, and goals.
Tips to increase the odds of success
- Bring a full medication list and, if requested, medical clearance.
- Optimize general health (reasonable diabetes control, smoking cessation, nutrition). Smoking notably raises implant failure risk — quitting improves outcomes.
- Choose an experienced implant dentist or prosthodontist who treats older patients and coordinates with medical doctors.
- Maintenance plan: daily hygiene, professional cleanings, and a night guard if you grind your teeth.
- Ask about alternatives (implant overdentures, fixed hybrid prostheses, or well-fitted conventional dentures) if full implants are cost-prohibitive.
Conclusion
Dental implants are a real, evidence-based option for many seniors: modern implants show high survival rates even in older populations, and age by itself is not a contraindication. That said, seniors often face unique factors — bone health, medications (such as bisphosphonates), chronic conditions, and insurance or financial limitations — that require careful planning. Talk frankly with your qualified dentist in Scottsdale and your medical team, weigh the benefits vs. the costs, and choose a treatment path tailored to your health and lifestyle. With good planning and follow-up, implants can restore comfort, chewing ability, and confidence for many older adults.
FAQs
- How long do dental implants last?
With proper care and oral hygiene, the titanium implant post itself can last a lifetime. The crown attached to the implant typically lasts between 10 to 15 years before needing replacement due to normal wear and tear.
- Is the dental implant procedure painful?
The procedure is performed under local anesthesia, so you will not feel pain during the surgery. Patients typically report some soreness or discomfort for a few days afterward, which is usually managed with over-the-counter pain relievers or prescription medication.
- Will my dental implants look and feel like natural teeth?
Yes. Implants are fixed permanently in your jaw, eliminating the movement associated with dentures. The crown on top is custom-made to match the color, shape, and size of your existing teeth, making them virtually indistinguishable from a natural, healthy tooth.
- How long is the recovery process for dental implants?
Initial healing takes about 1 to 2 weeks, but the crucial process is osseointegration—when the implant fuses with the jawbone. This biological fusion can take anywhere from three to six months. Only after this process is complete can the final crown be placed.
- Can I get dental implants if I have osteoporosis or wear dentures?
Osteoporosis is not an automatic disqualifier, but your doctor will assess your overall bone health, possibly requiring a bone density scan. Many seniors who currently wear dentures are excellent candidates for implants, particularly for implant-supported dentures (such as All-on-4), which are far more stable and comfortable than traditional removable models.